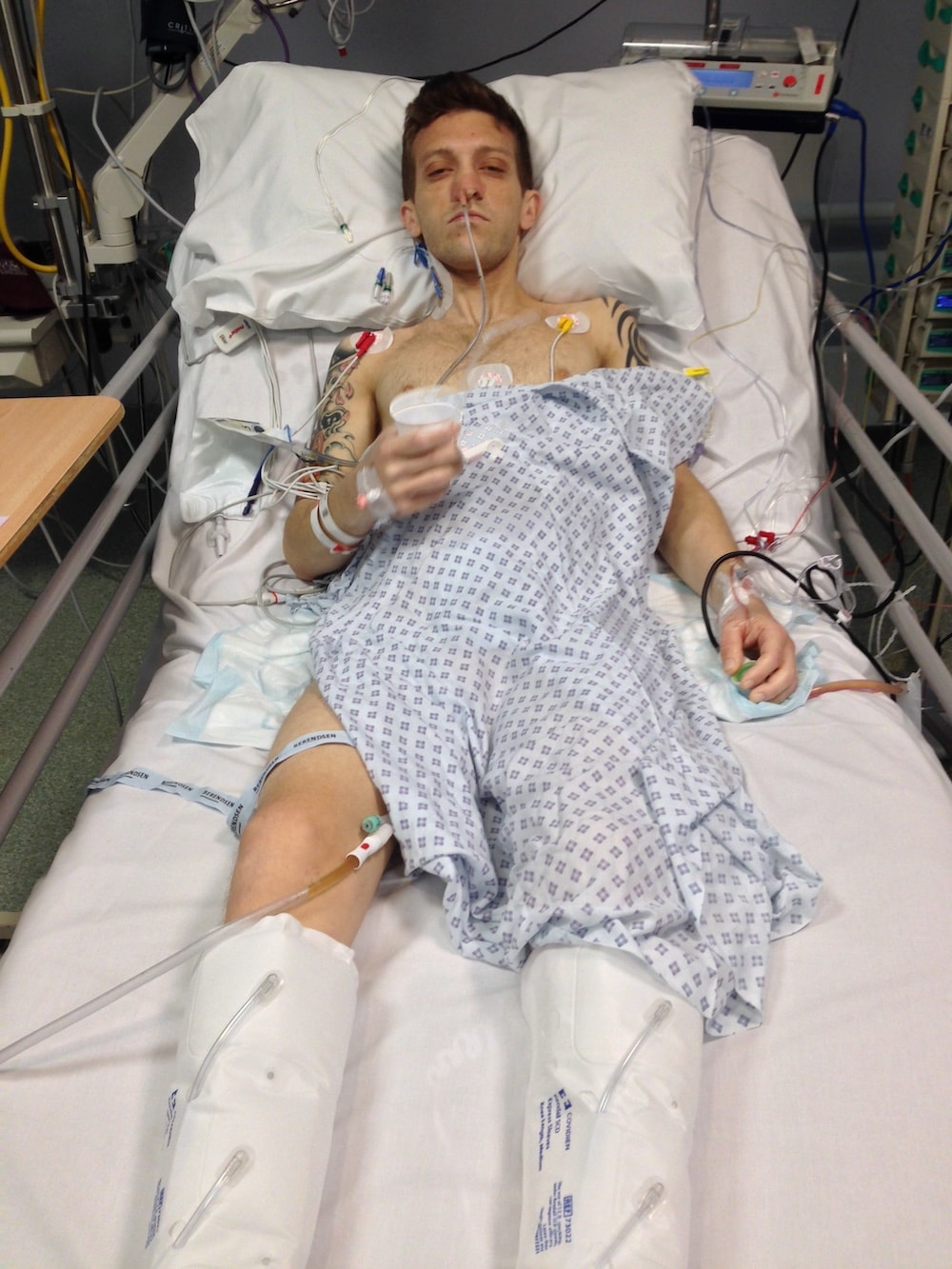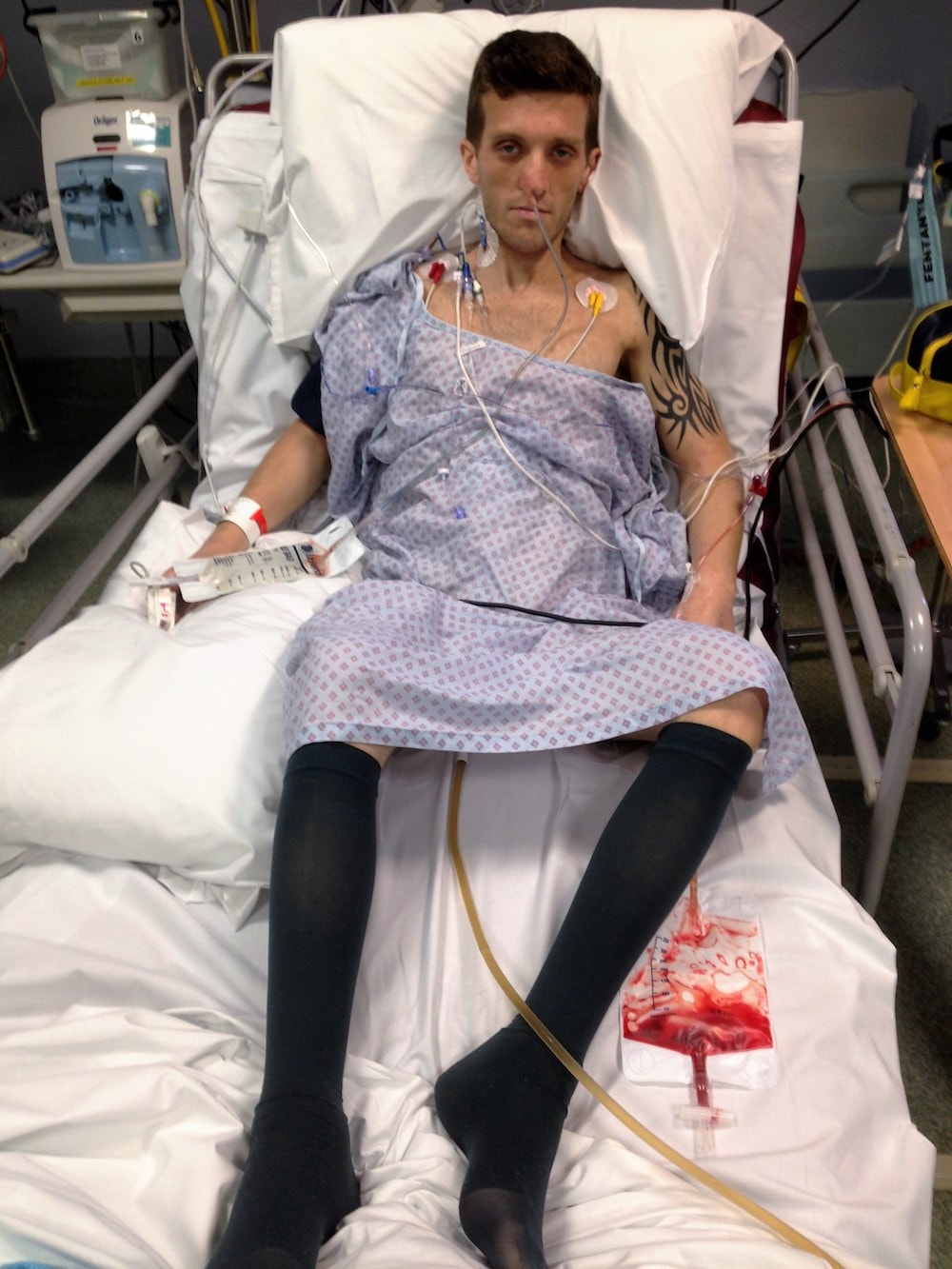
Rob Kirby’s extraordinary battle with ulcerative colitis is a testament to hope and resilience
I have ulcerative colitis, which affects the large intestine.
It’s an inflammation of the bowel, so ulcers will form on the lining of your bowel. They bleed, they’re really painful, and they stop you absorbing nutrients, so you get dehydrated and you lose weight, and because you’re bleeding you probably get anaemia as well. It makes you go to the bathroom quite frequently, and you’re probably sick.
When I was 16, at college, I used to get cramps, but dismissed them as tummy aches. They would pass after a few days and I’d forget about it. I went to Tenerife to celebrate my 21st birthday with my best friend; two young guys going crazy, and halfway through I was in so much pain that when I got home I went straight to A&E. They did an endoscopy and I was diagnosed with ulcerative colitis. It was 2005.
I remember reading this leaflet saying one in four people diagnosed with UC could end up with a colostomy bag. That’s all I was fixated on. I didn’t want surgery, but I was also in denial. I was very scared. I just buried my head. I did some intense treatments, things like steroids, really powerful drugs that boost your ability to repair, but the high doses can put you at risk of heart attack too.
It worsened over time. The drugs weren’t working. At this point I was doing enemas where you have to inject a baby’s bottle worth of steroids into your backside every night. I didn’t know how to do it. I’d lie on the bathroom floor and my wife Shelly would help me. You know, we’re not medical professionals, we’re two young twentysomethings. We didn’t know anything. I agreed to trial a drug called Infliximab. I was having infusions every eight weeks, where I’d go to hospital and they’d administer half a litre of this stuff. The drug was powerful, and being administered through the vein.
I went to theatre. I remember lying on the bed, crying, and they put me to sleep. I woke up and thought my body was on fire
I still went to work every day. I didn’t want to give up things I could control, like my job. That was very important to me. There are times I probably shouldn’t have gone, but I’m an analyst and I have a very analytical way of thinking. Ulcerative colitis has always been a competition to me: am I winning at this moment or am I losing? It’s very black and white. During this period I was also put on anti-depressants, and I still take them today.
Also, my best friend was killed while all this was going on. It wasn’t his fault and I didn’t deal with it very well either. That was a massive shock. And we were being evicted from our rented house. Lots and lots of things mounted up really quickly.
I did go to counselling. I sourced my own counsellor, and just by chance I found somebody where I was working who does it outside of work. She was incredible. I learned to concentrate on what was important.
One day I turned up to hospital and they said, “We’re not treating you today; the funding on Infliximab has been cancelled.” They wanted me to go to theatre there and then. I was at a critical level. They didn’t want me to leave hospital.
I begged and pleaded with the surgeon to let me go home and speak to my wife. She was maybe three months pregnant with our son, Alfie. I didn’t want to go to surgery without seeing my wife. Try and understand, they were talking about removing all of my large intestine, putting a colostomy bag on me, and then only after the surgery would they know if the bag could be reversed.
I was very scared. Would I survive? Because it was life-saving surgery. I went to theatre. I remember lying on the bed, crying, and they put me to sleep. I woke up and thought my body was on fire. The pain was just incredible. I’ve since learned that I’m allergic to all painkillers, so no morphine, tramadol or codeine. It was coming back to the winning and losing thing again, and I was losing.
I had bruising from the top of my chest down to my private parts. Everything hurt. But I wanted to be self-sufficient. I wanted to take the bag off, clean myself, and put a new bag on before they would release me from hospital. Your intestine actually protrudes through your skin like a five pence piece. I had no idea. The first time I saw that, I nearly passed out. I wasn’t prepared to see that. But the next day, I decided to do it myself.
Sarah Burton, from Frimley Park Hospital, Surrey, became my surgeon for the next five years. She was really good. I had to have another surgery where they built a new rectum out of my small intestine and let that heal. And then a third surgery. My son had been born by that point. I was told not to hold my baby because he was too heavy for me. F*ck that. I’m not listening to that. I’m not going to get this chance back, so I ignored their advice because it just seemed ridiculous.
But that wasn’t the end of it. Eventually I had 13 surgeries.
I had adhesions inside, so where they’d cut me on the inside, things were sticking together and causing obstructions in the bowel. I’ve had very invasive surgery. After one, I went home after five days but then within 24 hours I was back in hospital because my bowel had gone to sleep. At one point, I had a 34-inch waist but only weighed eight stone. I had a distended stomach. My rectum had split and the waste was leaking into my body, so I had more emergency surgery.
Throughout all these surgeries, I had other scary situations – a suspected heart attack (misdiagnosed), suspected liver failure (my liver reacts to medication), and a suspected cancerous lump (which turned out to be scar tissue).If my wife Shelley and our son Alfie weren’t here, I would have given up. Definitely
Finally, my surgeon said, “I don’t think there’s anything more I can do for you.”
I was sent to St Mark’s Hospital in Harrow, London, and was referred to Professor Sue Clarke, who is recognised as being the best in the world. She decided to take me on. Sue gave me three options: take everything out and have a permanent bag; try to fix what’s there, which isn’t an option; or remove the bad stuff and see if there’s enough left to build a new rectum. I didn’t want a bag, so I went for the most difficult option.
The surgery took place on 9 May, 2015. I was in intensive care for a few days because waste was leaking into my body. Then, in May 2016, I had surgery to take out the bad stuff. Sue could see it was horrendous. I was in surgery for nine hours. It was Sue and her assistant, another world-class surgeon. They managed to build me a new rectum, but they couldn’t connect it. I’m quite a small person. They couldn’t get their hands deep enough into my pelvis to connect what they’d done to my backside, so it looked like they were going to fail.
Sue telephoned a surgeon who was visiting the country, an Italian expert. He had this new technique and, luckily for me, he agreed to come in and conduct the surgery. Two surgeons work from the front through the stomach, and two work through the backside. They managed to get things connected. It was the first time this surgery had ever been done in the UK. They were thrilled.
When I woke up, I didn’t know what to expect. I’ve got all the good stuff but now I’ve got all this unknown stuff too. But everything worked out. I function normally now. I’ve put on weight. I don’t have pain. And I don’t go to the loo as much. Seriously, I don’t know how I got from there to here.
One thing I do know; if my wife Shelley and our son Alfie weren’t here, I would have given up. Definitely. I was ready to go. I never thought I’d get better because after every surgery I’d had, something else would go wrong. I owe Shelley my life. I owe Sue my life. I owe everybody that’s worked on me my life.
Through this whole process it was really important to talk with my wife. We found that if I express to her how I’m feeling and she can express to me how she’s feeling, then we’re going to be okay. The same goes for my friends and family. If I get a hug, a simple human connection, then it’s enough for me to know that someone cares about me. And I’m going to do it for them. I’m not going to be selfish, and I’m not going to give up.
Further information about ulcerative colitis can be found on the NHS's website.