Travel blogger Helen Renners suffered with aches and pains for her entire life – it wasn’t until university that she realised it was something serious. But it hasn’t held her back. In fact, she’s currently backpacking around the world

Helen Renners
As I write this, I’m sitting in the jungle in south Sri Lanka, in the first week of my 12-month solo backpacking trip around Asia and Australia. This time last year I could barely get out of bed. I would turn off my phone and shut myself away from the world for days at a time. My self-esteem was low and my anxiety was crippling. It became a vicious circle I didn’t know how to break out of.
As a child, I would constantly have a swollen, sprained ankle or wrist. I’d never remember exactly how it happened, but I would find myself
in so much pain that I couldn’t put my weight on one foot, or my wrists would ache as though I had fallen and landed badly on them. It became a running joke in my family that I was “spraining my ankle” to avoid PE.
When I was 19 and at university, I joined the gym for the first time. I’d run on the treadmill and for the next few days my feet would be swollen and achy. At 20, I went to Thailand with some friends and my feet would ache after long days of exploring. In the mornings, my hands were so painful that I wouldn’t be able to unscrew a bottle of water or have the strength to lift a pot of tea. When I got home, I spoke to my mum and she decided I needed to see a doctor.
My GP said my hands and feet looked normal and sent me away. But when I went back to the gym and started running, my feet instantly swelled to the biggest cankles I’ve ever seen! I went straight back to my GP to show them what had happened. They sent me for blood tests and told me to avoid doing anything that would have any impact on my feet – no more running, no jumping, and no wearing heels!

Helen Renners
The tests came back and I was told I had a ridiculously high erythrocyte sedimentation rate (ESR) in my blood – the highest they’d ever seen in someone of my age.
ESR indicates the level of inflammation in my joints. It had been a week since I’d been told to avoid anything causing impact on my feet, so they sent me for more blood tests to compare with my initial ones. There wasn’t much difference between the two, despite the physical appearance of swelling going down. My doctor decided it was highly likely I had rheumatoid arthritis and would need to be referred to a specialist.
I was really freaked out; wasn’t arthritis what old ladies got when they needed their hips replaced?! I wasn’t even 21 yet.
It took a long time for my appointment to come through, and when it finally came around, they took some blood, poked and prodded me, and took some kind of bright orange goo out from behind my knee caps, which, being scared of needles, was pretty traumatic. After several hours, they decided there wasn’t much inflammation in my blood anymore so there was nothing for them to work with. I was discharged – great!
I got used to adapting my life to avoid aggravating my joints, and sort of forgot about it. I moved to London when I turned 23 and started back at the gym. But one morning I woke up and couldn’t lift the duvet with my hands. My fingers were bent and I couldn’t straighten them. When this didn’t stop after a few weeks, I went to see my new doctor, and after hearing about my history, he sent me straight to the nurse for blood tests there and then.
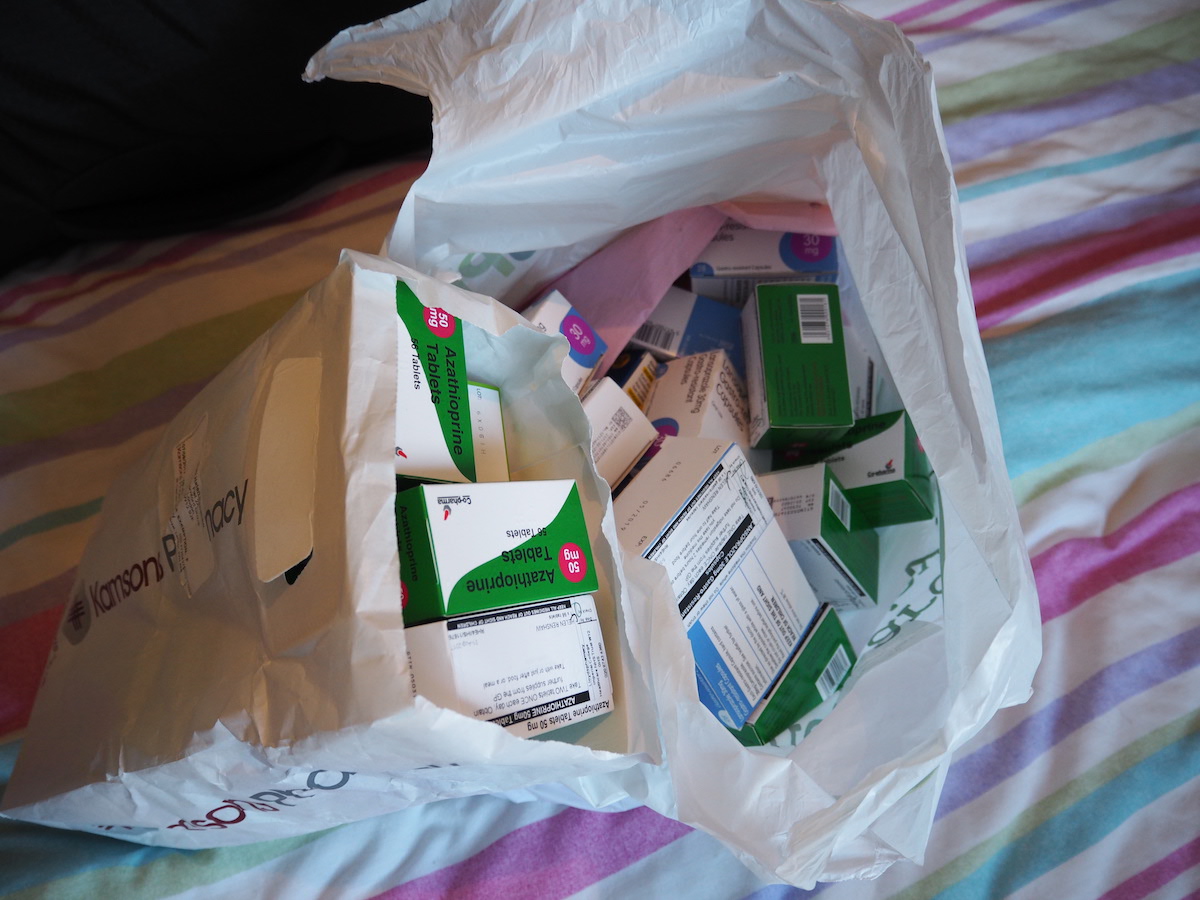
Helen's medication
Within two weeks, I’d been sent for an appointment with a specialist in Charing Cross Hospital. It was all so fast; I arrived for my appointment and was weighed, asked for a urine sample, had more blood tests, and was sent for a lung X-ray. I remember being rushed around different departments in the hospital and not having a clue what was going on.
Eventually I saw the doctor, who said: “You have severe rheumatoid arthritis and we need to start you on medication immediately to stop any further damage to your joints. Once you start this treatment you can’t just stop – we’ll have to wean you off to avoid damaging your organs.”
I burst into tears. I was so overwhelmed by what was going on and didn’t really have any time to process it.
One morning I woke up and couldn’t lift the duvet with my hands. My fingers were bent and I couldn’t straighten them
Once I started on the medication, things still didn’t clear up quickly. I had extreme side effects that made me really poorly. Weight loss, weight gain, hair loss, a swollen face, tiredness, skin rashes, hyper pigmentation in my skin, nausea – I went through it all. Months would go by where they would adjust my meds or swap me onto new ones and I still wouldn’t feel well.
Some meds worked better than others, but I still didn’t feel 100% and I kept telling my doctors this. As far as they were concerned though, everything was “probably as good as it [was] going to get”.
For me, this answer didn’t cut it. I researched the effects of nutrition on your health and started to cut down on sugar and wheat. This made a slight difference, but I was still suffering with anxiety and aches I couldn’t explain – they didn’t feel the same as the pain in my joints from the arthritis.

Helen's medication
I stood my ground and kept going back to the hospital. I knew my body wasn’t 100% and that they must be missing something. Last year, when I was at my lowest – exhausted, stressed, and confused about what was happening to me – it made me feel like I was going insane! Eventually though, the doctors found that I also have systemic lupus erythematosus.
Lupus and rheumatoid arthritis have very similar symptoms, and it was the early symptoms of lupus that had been put down to side effects of the medications.
I wasn’t happy to hear I had a second autoimmune disease to contend with, but I was so relieved to finally find out why I was feeling so horrific. My personality had changed so much; I was reclusive because I didn’t have the energy to explain to people how I felt. Autoimmune diseases aren’t visible, and in my experience, they can make you feel very lonely. It can be embarrassing not to be able to do everything your friends can easily do, and you don’t want to keep reminding them because you want to carry on as normal.
Once I was on the correct medications, I quickly began getting back to my old self. My friends were amazing. I explained what was happening and why I’d been off the radar, and instantly regretted not letting them know sooner.
I always wanted to travel the world, but because of my condition the doctors wouldn’t recommend it while my health was unstable. This year, my specialist finally agreed it was safe for me to travel. He prescribed me with six months’ medication, on the condition I go for blood tests once a month while I’m away and email him the results.

Helen with friends
If you’re struggling with an autoimmune condition, or anything similar, you honestly don’t need to suffer in silence. Speak to your friends, your family and your doctors. If you’re given a diagnosis but still don’t feel 100%, keep going back and asking for more answers – you know your body better than they do. It took six years for medical professionals to find out I had lupus as well as rheumatoid arthritis, and since I found out I’ve been so much better off.
It can be a long process but it does get better, and it shouldn’t stop you doing anything you want to do. You may have to adapt things slightly, but you can still live a happy life. I know this because that’s what has happened to me. I’m setting out on an adventure I always dreamt of but never thought possible, and am so excited for the future!
Helen now shares her experiences of travelling with autoimmune conditions on her blog, beachdontkillmyvibe.co.uk
Helen is an inspirational young woman. Her story illustrates the importance of keeping the lines of communication open, even when we may find it hard to be heard. Now, her doctor is helping her fulfil her ambitions. She reminds us that help is there from both friends and professionals. Reaching out is the first step toward achieving our dreams, just as Helen is today!

Join 100,000+ subscribers
Stay in the loop with everything Happiful